| PYQ Relevance[UPSC 2015] “Besides being a moral imperative of a Welfare State, primary health structure is a necessary precondition for sustainable development.” Analyse.Linkage: This PYQ is important for understanding GS-2 health governance and social sector issues. The PYQ links with the theme of preventive healthcare and helps analyse the transition from a curative healthcare model to a preventive and wellness-oriented approach in India. |
Mentor’s Comment
India’s healthcare discourse is increasingly shifting toward preventive healthcare. This is driven by a rapid rise in non-communicable diseases (NCDs), mounting healthcare costs, and evidence from large-scale health assessments such as the Apollo Hospitals Health of the Nation Report 2026.
Why is India’s healthcare success insufficient without preventive health culture?
- Curative Bias: India has built strong institutions for treatment, trained clinicians, and advanced medical infrastructure. However, the system responds more effectively to illness than preserving wellness.
- Health Perception Gap: Society often treats health as something to recover after illness rather than protect daily through preventive practices.
- Preventive Deficit: National health outcomes remain constrained because healthcare systems predominantly intervene after disease onset. This reduces opportunities for reversal.
- Civilisational Shift: Preventive healthcare requires moving from episodic treatment to continuous self-care, involving individuals, families, and communities.
How serious is India’s burden of chronic diseases?
- NCD Burden: Non-communicable diseases (NCDs) such as heart attacks, strokes, cancer, and diabetes have emerged as the leading causes of death in India, surpassing infectious diseases.
- Scale of Crisis: 270 million Indians live with chronic disease, while many remain unaware of their condition until the disease significantly progresses.
- Silent Disease Burden: Many chronic conditions remain asymptomatic in early stages, leading to delayed diagnosis and higher treatment costs.
- Demographic Threat: Chronic diseases increasingly affect working-age populations, threatening India’s demographic dividend.
- Economic Consequences: Preventable illness reduces workforce productivity and diminishes the contribution of individuals during their economically productive years.
Why is the age group of 30-40 years a critical intervention window?
- Turning Point: The Apollo Hospitals Health of the Nation Report 2026 identifies the decade between 30 and 40 years as a critical phase where metabolic and cardiovascular risks begin to emerge.
- High Vulnerability: Individuals in this age group are typically engaged in career-building and family responsibilities. This makes health deterioration economically costly.
- Disease Progression: By the age of 40, a significant proportion of people cease to be disease-free.
- Awareness Deficit: Most individuals avoid preventive healthcare because symptoms are absent, despite underlying risk accumulation.
- Missed Opportunity: Delayed action often closes the possibility of early reversal of lifestyle diseases.
Can preventive healthcare reverse India’s disease burden?
- Early Detection: Timely diagnosis through screening facilitates identification of diseases before complications emerge.
- Lifestyle Correction: Behavioural modifications involving diet, physical activity, stress management, sleep, and substance reduction can delay or reverse many chronic conditions.
- Sustained Monitoring: Periodic check-ups support risk identification and disease management before advanced progression.
- Biological Resilience: The human body demonstrates significant recovery potential when intervention occurs at early stages.
- Limited Opportunity Window: The editorial stresses that the “window of prevention” does not remain permanently open, necessitating early action.
Why must preventive healthcare become a national philosophy rather than a medical programme?
- Self-Stewardship: Prevention requires citizens to treat health as a personal responsibility rather than solely a medical issue.
- Behavioural Transformation: Sustainable outcomes require routine practices rather than one-time interventions.
- Family-Level Impact: Health choices affect not only individuals but also dependents and future generations.
- National Productivity: Economic growth depends on a healthy and productive population.
- Human Capital Formation: Preventive health strengthens longevity, vitality, workforce participation, and social well-being.
What structural barriers prevent India from adopting preventive healthcare?
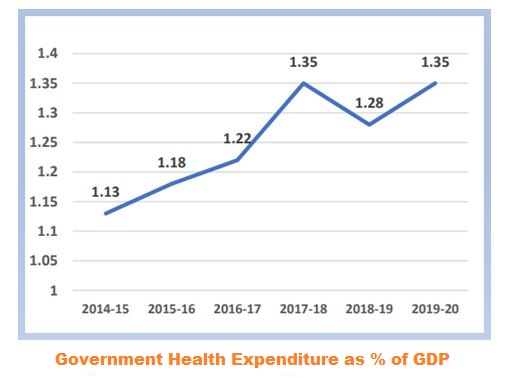
- Treatment-Oriented System: Healthcare financing prioritises hospitals and treatment over wellness and prevention.
- Low Health Awareness: Citizens often seek care only after symptom manifestation.
- Lifestyle Risks: Urbanisation, sedentary habits, unhealthy diets, stress, tobacco use, and pollution aggravate disease burden.
- Limited Screening Culture: Routine annual health assessments remain uncommon.
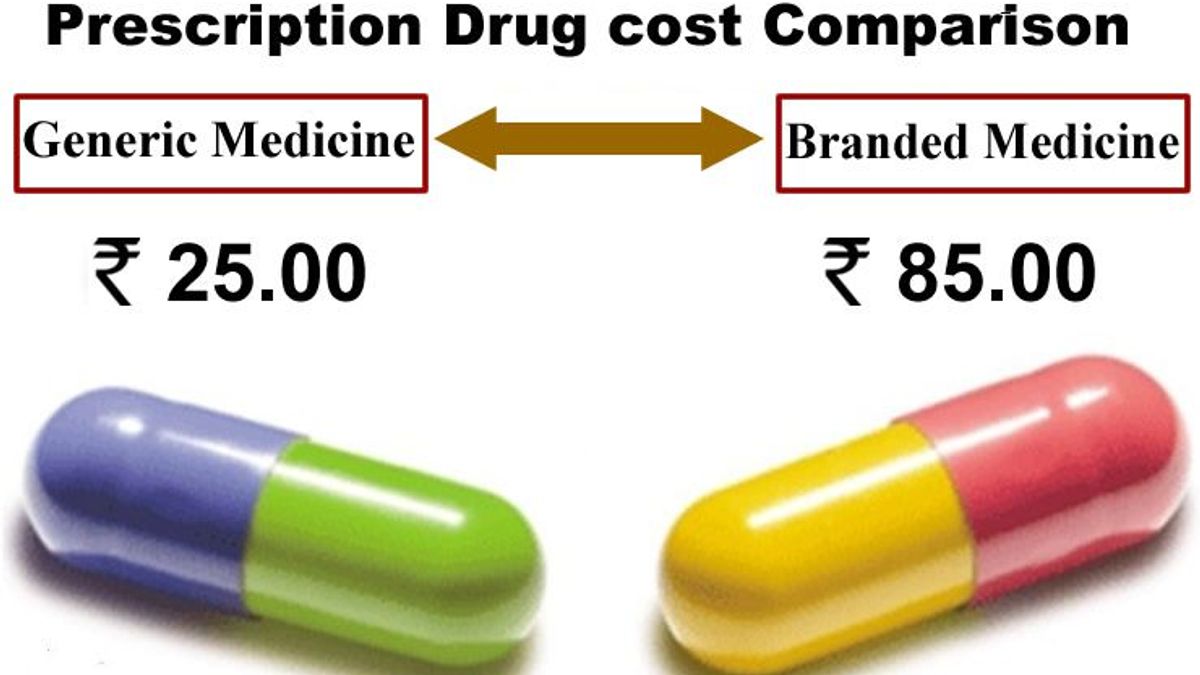
- Out-of-Pocket Expenditure: High medical costs discourage early diagnosis.
How can India build a preventive healthcare ecosystem?
- Routine Screening: Institutionalise annual health assessments, particularly for adults above 30 years.
- Primary Healthcare Strengthening: Expand screening and wellness through Ayushman Bharat Health and Wellness Centres (HWCs).
- Health Literacy: Promote awareness regarding lifestyle diseases, nutrition, exercise, and mental health.
- Digital Health Infrastructure: Use digital records and AI-enabled diagnostics for early risk detection.
- Workplace Wellness: Encourage preventive screening in workplaces and institutions.
- School-Based Prevention: Embed nutrition, exercise, and health awareness in school education.
- Community Participation: Strengthen local wellness campaigns through panchayats and urban local bodies.
Conclusion
India’s healthcare journey must move beyond excellence in curing disease toward excellence in preventing it. A healthy nation depends not only on hospitals and doctors but also on everyday choices shaped by awareness, early intervention, and institutional support. Preventive healthcare is not merely a medical strategy; it is an economic necessity, a social responsibility, and a national developmental imperative.
















































































































































 Context
Context What is paediatric cardiac care?
What is paediatric cardiac care? What are the Reasons behind this worrisome situation?
What are the Reasons behind this worrisome situation? What should be approach for the treatment of Congenital Heart Disease?
What should be approach for the treatment of Congenital Heart Disease? Context
Context Facts on rabies
Facts on rabies  What is the issue?
What is the issue?  How can we prevent rabies in animals?
How can we prevent rabies in animals? Context
Context  Why is anaemia so high in the country?
Why is anaemia so high in the country? Why need iron fortification?
Why need iron fortification? Success story / value addition
Success story / value addition Context
Context  What are 4 pillars of public health?
What are 4 pillars of public health?  What are the hurdles in absorbing others as public health professionals?
What are the hurdles in absorbing others as public health professionals? Context
Context  There is widespread inequity in healthcare
There is widespread inequity in healthcare  India’s lead role
India’s lead role Context
Context  Reasons for Persistence of
Reasons for Persistence of  Ongoing challenges in mental wellness regime
Ongoing challenges in mental wellness regime 
 Context
Context  The National Digital Health Mission
The National Digital Health Mission Significance of digital health
Significance of digital health  Context
Context  A systemic approach to reforming healthcare system in the country needs
A systemic approach to reforming healthcare system in the country needs




































