Healthcare is LITERALLY the talk of the town right now. But for all the wrong reasons. Whether it is the lack of beds/ventilators or high cost of treatment, COVID has amplified our present deficiencies. Like rest of the world, Indians are for the first time so singularly focused on healthcare and public health amid this pandemic. And everyone suddenly wants to fix healthcare!

Confucius, it is said, once observed, “a seed grows with no sound, but a tree falls with huge noise. Destruction has noise, but creation is quiet”. As we all know, the world is at a crossroads. With COVID-19, many of our beliefs and the systems we follow are bound to change OR even get collapsed!
Healthcare in India: A Background
- The Indian Constitution has incorporated the responsibility of the state in ensuring basic nutrition, basic standard of living, public health, protection of workers, special provisions for disabled persons, and other health standards, which were described under Articles 39, 41, 42, and 47 in the DPSP.
- Article 21 of the Constitution of India provides for the right to life and personal liberty and is a fundamental right.
- Public Health comes under the state list.
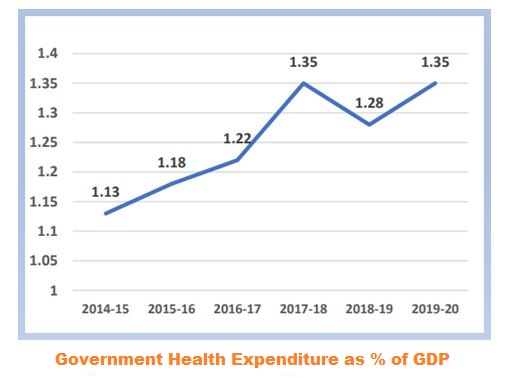
- India’s expenditure on healthcare has shot up substantially in the past few years; it is still very low in comparison to the peer nations (at approx. 1.28% of GDP).
All-time Paradoxes of Indian Healthcare
(1) Healthcare is a fundamental right, but it is not fundamentally right in India:
The Supreme Court has held healthcare to be a fundamental right under Article 21 of the Constitution.
The expenditure on healthcare is one of the lowest in the world, lower than nations with similar economic growth rates. Though our economy has grown robustly post-liberalization, investment in healthcare has consistently hovered around 1% of the GDP. In the 2020-21 Budget, it was 1.02% of overall expenditure.
(2) Sector attracts investments, but delivery remains contentious:
India’s healthcare sector has attracted a steady stream of investments, albeit at the higher end of the value chain — the secondary & tertiary care. Lack of penetration, inflated billing, opaqueness in diagnosis, and poor quality of service has ensured that most Indians get treated below the standards prescribed by the WHO.
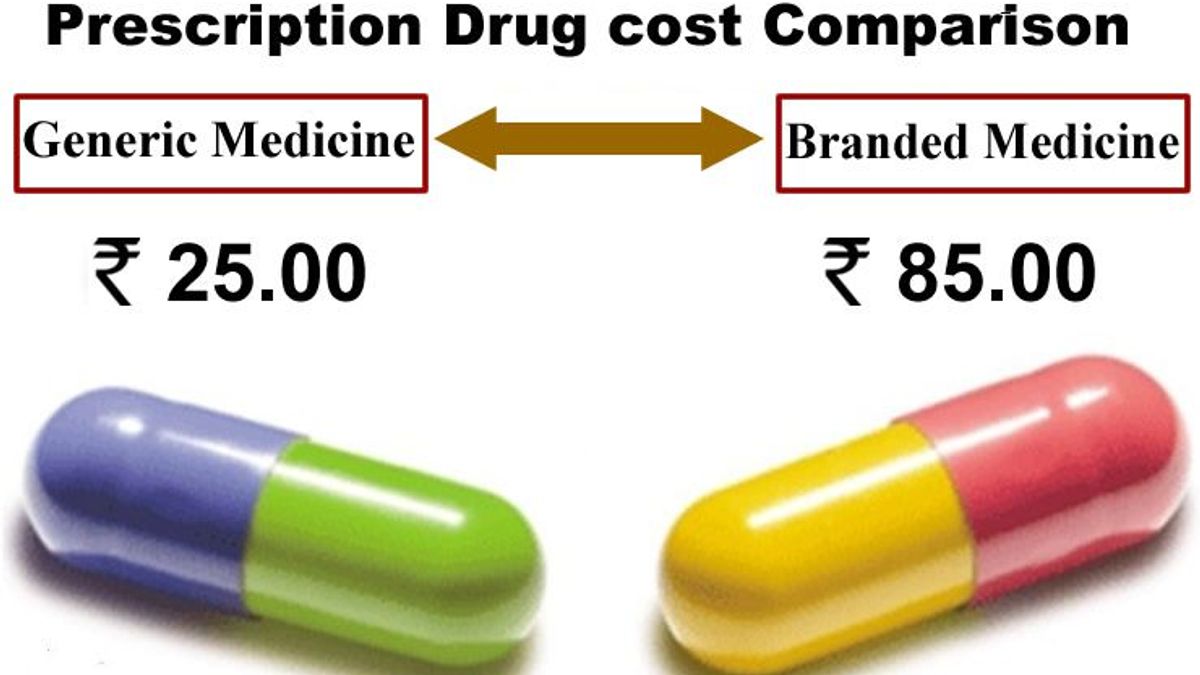
(3) Among the cheapest in the world, yet unaffordable for most locally:
Healthcare in India is cheap. For example: Compared to India, the cost of a knee replacement treatment is over twenty times more in the US and double in Malaysia. Yet India has one of the world’s highest rates of out-of-pocket spending in healthcare. There are millions in India who cannot afford these procedures in their own country.
(4) Less than one doctor for 1,000 patients, but medical tourism booms:
- India treated 3.6 lakh foreign patients in 2016 and the country’s medical tourism market is expected to grow to $7-8 billion by 2020.
- The doctor-patient ratio in India is less than the WHO-prescribed limit of 1:1000. There is a dearth of medical schools and clinicians.
- Most hospitals in India are overburdened, understaffed, and ill-equipped. However, all this has not prevented the private healthcare sector to establish sophisticated medical tourism facilities on the plank of ‘world-class service at low cost’.
(5) Stark divergence in healthcare outcomes within the country:
Healthcare being a state subject, the healthcare outcomes have remained divergent based on the quality of the state administration. While North India is the most populated part of India, it has one of the most undeserved healthcare infrastructures in the country.
Is India prepared to face this pandemic?
- Current health infrastructure in India paints a dismal picture of the healthcare delivery system in the country.
- Public health experts believe that India is ill-equipped to handle such emergencies. It is not prepared to tackle health epidemics, particularly given its urban congestion.
- Post unlock, the spread is at a galloping rate.
- The slum clusters all around the cities and the unhygienic growth, poor waste disposal system will only aggravate the situation.
History shows us that “blame” has been a standard human response during pandemics.
These are some issues surfaced during this pandemic ………..
(1) Poor Infrastructure
- In the 2019 Global Health Security Index, which measures pandemic preparedness for countries based on their ability to handle the crisis, India ranked 57, lower than the US at 1, the UK at 2, Brazil at 22, and Italy at 31.
- This is well revealed through indicators like hospital beds per 1,000 people.
- As per the OECD data available for 2017, India reportedly has only 0.53 beds available per 1,000 people as against 0.87 in Bangladesh, 2.11 in Chile, 1.38 in Mexico, 4.34 in China, and 8.05 in Russia.
(2) Fewer doctors per thousand
- The WHO mandates that the doctor to population ratio should be 1:1,000, while India had a 1:1,404 ratio as of February 2020.
- In rural areas, this doctor-patient ratio is as low as 1:10,926 doctors as per National Health Profile 2019.
(3) Denial of healthcare
- Despite private hospitals accounting for 62 percent of the total hospital beds as well as ICU beds and almost 56 percent of the ventilators, they are handling only around 10 percent of the workload.
- Private hospitals are reportedly denying treatments to the poor. Cases of overcharging patients are also being reported in private hospitals.
- This is seen in Bihar, which has witnessed an almost complete withdrawal of the private health sector and has nearly twice the bed capacity of public facilities.
(4) Discrepancy in Testing
- India continues to test less than it should in a post-lockdown scenario where testing is one of the most obvious ways to flatten the curve.
- The Supreme Court, after ruling on April 8 that private labs should conduct free testing, modified its decision five days later to fix the rate of one of the most dependable tests at Rs 4,500.
(5) Negligence for mental healthcare
- The tragic death of an actor and the gloom of the Covid-19 pandemic have led to much-needed conversations on mental health in the country.
- Mental health problems were already a major contributor to the burden of illness in India which usually gets unnoticed.
- The widespread anxiety due to lockdown has frustrated the laborers, farmers, and various vulnerable sections to a great extent due to the fear of impoverishment and loss of livelihoods.
Need of the hour: A tectonic overhaul
(1) Universal health coverage
- Access to healthcare in India is not equitable—the rich and the middle class would survive the COVID-19 or any other crisis but not the poor.
- As part of the SDGs, all countries have pledged to deliver universal health coverage (UHC) by 2030.
- This includes India. But, sadly, nearly 50 percent of the world’s population lacks essential health services.
- If any good comes out of this crisis, then it will be India waking up to the reality that investing in health is not a luxury. It is a basic need.
(2) Increasing healthcare professionals in numbers
- India has handled the COVID-19 pandemic exceptionally well. However, considering the rise in the number of infections, India is in dire need of more medical staff and amenities.
- If India wants to achieve a 1:1,000 ratio, it will need an additional 2.07 million doctors by 2030. For this, the government needs to increase its spending on the health sector.
- It needs to aid attempts at constructing new medical institutes.
(3) Revamping medical education
- If the government wants to stay successful in fighting the COVID-19 pandemic, it needs to rapidly build medical institutions and increase the number of doctors.
- Once COVID-19 is under control, we need to consider the psychological and professional impact of the pandemic on medical professionals.
(4) Helping the downtrodden
- How the poor are going to manage without, or even with, any government insurance scheme is a big question.
- Rather than dumping them on government hospitals only, the private hospitals should be held accountable to take on their treatment.
- They can make up for the loss by cross-subsidizing treatments of patients with premium insurance policies.
(5) Enhancing pandemic preparedness
- With COVID-19 we risk once again falling into the trap of a narrow vertical disease-specific approach.
- Decades of global health experience have revealed the limitations of narrow “vertical” disease-based programs.
- However, there is a need for recognition to combine vertical programs with “horizontal” health system strengthening.
(6) Optimum use of technology
- The COVID-19 crisis has elevated the importance of digital tools and e-health.
- There is a growing use of mobile apps, online consultations, e-pharmacies, and other tools.
- These are all welcome and must be leveraged.
(7) Looping-in private players
- For too long, India has allowed the private health sector to grow, with little regulation.
- The lack of alignment between the public and private sectors has been clearly exposed to COVID-19 testing and treatment in India.
- Time is ripe to loop in private players and promote the industrialization of health-sector.
(8) Learning from the successes
- With crumbling health infrastructure due to overburden, India’s preparedness for handling this epidemic has become a major challenge.
- The world along with India being no exception has responded with extraordinarily aggressive measures such as phased lockdowns, Bhilwara Model, Pathanamthitta Model, Taiwan model, etc.
- The success of these models is attributed to various best practices which are were implemented days before the thought of nationwide lockdown was incepted.
Kindly refer for various success models:
[Burning Issue] Success stories in handling COVID-19 crisis
Way Forward
- The aerial spread of the pandemic post unlock poses a threat of rapid dissemination but it can still be contained with an efficient response that combines effective public health, microbiological, clinical, and communication responses.
- While our laboratory network has improved somewhat, but much needs to be done to improve the community facing primary health services and risk communication to the public.
- Kerala’s success in responding swiftly and smartly to the outbreak should be a role model for other states.
Conclusion
India’s healthcare system is too small for such a large population. There seems to be a long battle ahead. The public healthcare system cannot be improved overnight. The country needs all hands on deck during and after this crisis—both public and private sectors must work together and deliver universal health coverage for all citizens.
Ultimately, the onus of governance always rests with the government, which needs to set standards, invest resources, ensure quality, and strategically purchase services from the private sector, as needed.

















































































































































 Context
Context What is paediatric cardiac care?
What is paediatric cardiac care? What are the Reasons behind this worrisome situation?
What are the Reasons behind this worrisome situation? What should be approach for the treatment of Congenital Heart Disease?
What should be approach for the treatment of Congenital Heart Disease? Context
Context Facts on rabies
Facts on rabies  What is the issue?
What is the issue?  How can we prevent rabies in animals?
How can we prevent rabies in animals? Context
Context  Why is anaemia so high in the country?
Why is anaemia so high in the country? Why need iron fortification?
Why need iron fortification? Success story / value addition
Success story / value addition Context
Context  What are 4 pillars of public health?
What are 4 pillars of public health?  What are the hurdles in absorbing others as public health professionals?
What are the hurdles in absorbing others as public health professionals? Context
Context  There is widespread inequity in healthcare
There is widespread inequity in healthcare  India’s lead role
India’s lead role Context
Context  Reasons for Persistence of
Reasons for Persistence of  Ongoing challenges in mental wellness regime
Ongoing challenges in mental wellness regime 
 Context
Context  The National Digital Health Mission
The National Digital Health Mission Significance of digital health
Significance of digital health  Context
Context  A systemic approach to reforming healthcare system in the country needs
A systemic approach to reforming healthcare system in the country needs




































